Revenue Cycle Improvement Program (RCIP)
Nevada Rural Hospital Partners (NRHP) recognized that maintaining an effective revenue cycle is the bedrock of financial viability. The effectiveness of a hospital’s revenue cycle drives the entire hospital operation because the cycle is the source of the resources needed to maintain a successful facility. NRHP also recognized that to be effective the cycle must be viewed as a whole – success rests in how well the cycle is integrated. And finally, NRHP recognized that small hospitals need hands-on guidance, training, and implementation support. Our Revenue Cycle Improvement Program was specifically developed to enable small and rural hospitals to achieve optimal financial performance in an increasingly challenging financial and regulatory environment.
Our Concept
The outer cycle is possible only when the inner cycle is effective. A successful revenue cycle is a complex process involving many inter-related components. The graphic below illustrates these relationships and underscores the fact that the effectiveness of the component parts drives the ability to deliver services to patients – the outer cycle is possible only when the inner cycle is effective.
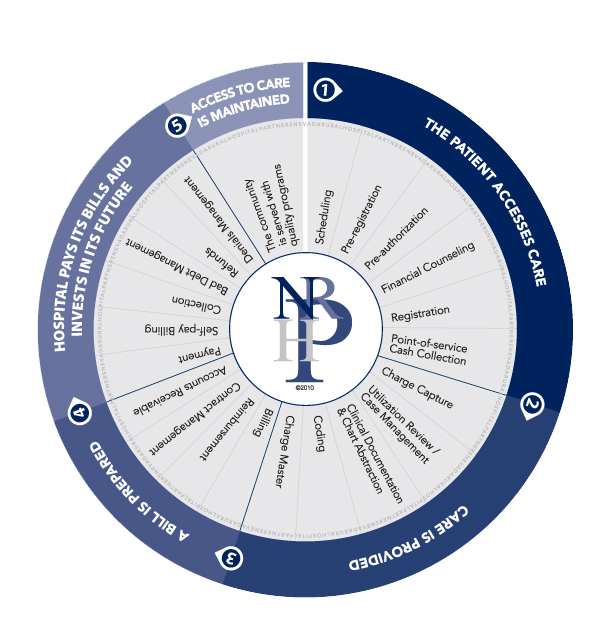
NRHP Revenue Cycle Wheel
NRHP categorizes the components of the revenue cycle as they related to patient access to care:
- Activities that support patient access to care, such as patient scheduling, pre-registration, preauthorization, financial counseling, registration and point of service cash collection;
- Activities that reflect the delivery of care from a financial perspective such as a charge capture, utilization review, documentation and chart abstraction, coding, and the maintenance of an accurate current charge master;
- Activities that generate an accurate bill for that care through billing, accounts receivable, receipt of reimbursement, and contract management;
- Activities that have to do with the receipt of payment including self-payment, collections, bad debt management, refunds and denials management; and,
- The utilization of those funds to continue to support the operation of the hospital and patient access to care.
Our Process
Applying our commitment to an integrated approach, our process typically includes:
- A detailed assessment of your revenue cycle (current state);
- A tailored definition of the desired future state taking resources and capabilities into account;
- A gap analysis including an evaluation of current policies, procedures, and forms;
- A transition plan that bridges current practice to the future state;
- Intensive hands-on implementation support in your hospital;
- Recommendations for external vendors if necessary, and assistance with RFPs and coordination of the vendors based on your needs;
- Benchmarking using core performance indicators, data gathering tools, and custom facility reports to help you measure and sustain progress; and,
- A period of intensive follow-up to support permanent improvement.
